There were several debates for the treatment and prognosis of unruptured VAD, and their optimal treatment has not been established. Because initial angiography was performed at least several days after the onset of the preceding symptoms, most of the VADs that were unruptured at diagnosis already had little risk for bleeding. In our analysis, most patients visited our institute after the acute stage. 7, 11, 13, 15, 21, 22) Those studies suggest that if 4 or more days pass without bleeding episodes, the prognosis of patient with unruptured VAD may be good. Some authors reported the interval between onset of preceding symptoms and bleeding episode. The diagnosis of dissecting aneurysm has been discussed by many authors based on angiographic findings such as "pearl and string" sign, 12, 16, 22) fusiform, 3, 19) linear defect, 4) true and false lumen (double lumen), 6) and retention of the contrast medium in the venous phase. But vascular wall MRI was used to diagnose in all patients. Conventional angiography was done at initial presentation only in 3 cases of acute onset. In our analysis, not all patients were diagnosed with conventional angiography. More studies are needed to verify the relationship between shape of VAD and its risk.Ĭonventional angiography has long been the gold standard in the diagnosis of VAD, since it can show the arterial lumen and allows extensive characterization of dissections of vertebral arteries. Many studies suggested that shape of aneurysm is related to the risk of rupture, but those in VAD are few. The shape of VAD was not significantly related to the outcome. All the patients had benign clinical outcomes. There were 5 patients with fusiform aneurysm, 1 with saccular aneurysm, and 1 with dumbbell-shaped aneurysm in our analysis. Most defects were located near the branching of the PICA 10 to 20 mm distal to the site of penetration of the dura mater, this may be related to the development of dissection at these site.Īccording to Kim et al., 8) the shape of VAD was not considerably related to the functional outcome. This type of VAD appeared as subarachnoid hemorrhage (SAH) and resulted in devastating disease with high mortality rates. It shows a widespread disruption of the entire thickness of the arterial wall with the formation of a dilated pseudo-aneurysm, which consisted of thin adventitia. The other type of VAD is full thickness disruption, the most common type. In this analysis, no patient showed the evidence of vertebrobasilar artery ischemia on radiologic evaluation. Most of this type showed tapered narrowing or double lumen, and presented as vertebrobasilar artery ischemia with a fair outcome. The intramural hematoma is located within the layers of the tunica media, but it may be eccentric, either toward the intima or toward adventitia. The tear allows blood under arterial pressure to enter the wall of the artery and form an intramural hematoma. The internal elastic lamina is weakened and disrupted with aging and long-standing hemodynamic stress. Dissections of vertebral arteries usually arise from an intimal tear. The first type of VAD is partial thickness disruption. Mechanical stress to the arteries may be even caused by sudden head rotation in daily life. Traumatic VAD means VAD due to major blunt or penetrating traumas like motor vehicle accidents, falls or penetrating injuries. Spontaneous VAD is the term used to describe vertebral dissections that do not involve blunt or penetrating trauma as a precipitating factor. 1, 12) VAD can occur spontaneously or after blunt or penetrating trauma. VAD is a relatively uncommon disease, however, its clinical course is known to be somewhat devastating, with estimated mortality to be 17-46%. No patient experienced neurological deterioration due to subarachnoid hemorrhage or vertebrobasilar ischemia during follow-up period. Others show no interval change of size or shape of aneurysm during the follow-up period. In one of them with unstable aneurysm, the aneurysmal size decreased in the last follow-up study. They were also managed with antihypertensive and analgesics medications. They were evaluated more frequently using CTA, roughly weekly base. Another two patients showed unstable state of aneurysm due to change in shape during the follow-up period. One of them showed the complete disappearance of aneurysm. 
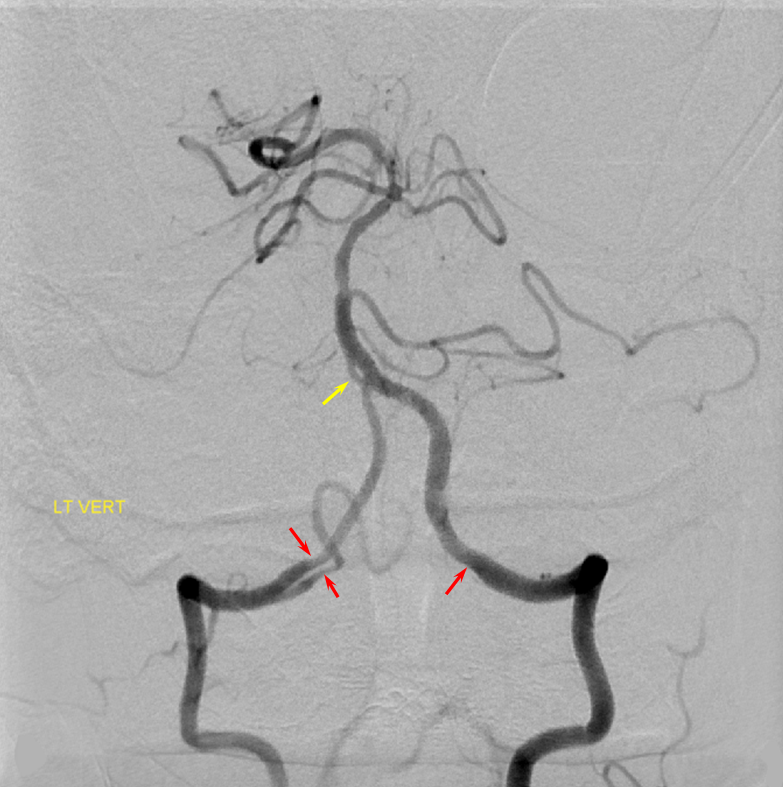
In two patients, aneurysms showed getting smaller during follow-up period. No one had VAD below the origin of PICA (proximal vertebral artery). 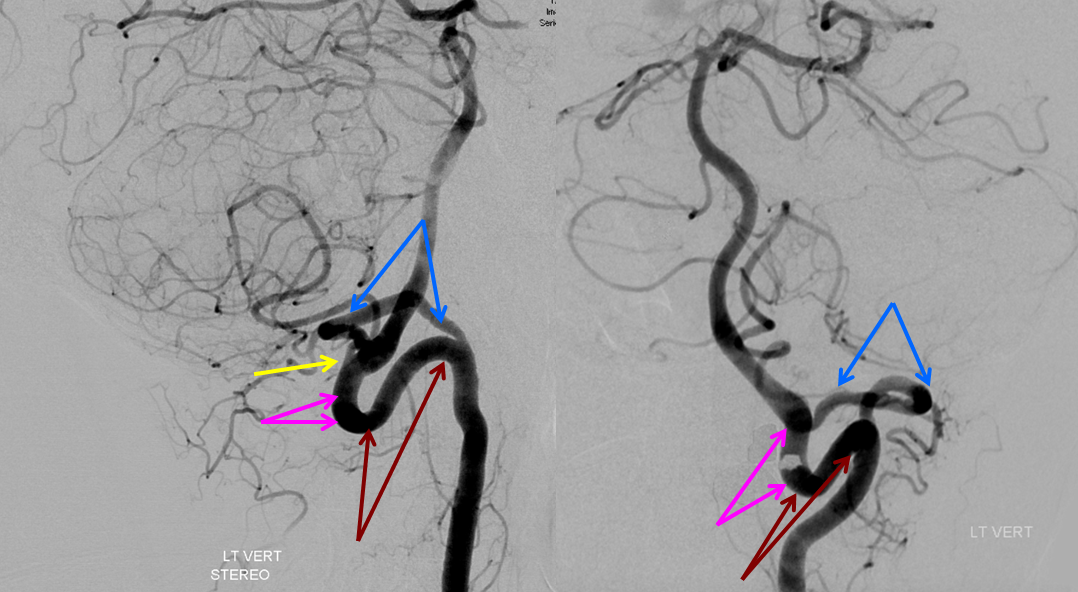
Clinical characteristics of the patients and location and shape of aneurysmĪt the time of diagnosis, 5 VAD were categorized as distal vertebral artery dissection above the origin of posterior inferior cerebellar artery (PICA)(distal vertebral artery), 2 involving the PICA. 
0 Comments
Leave a Reply. |
 RSS Feed
RSS Feed
